|
|
|
|
TRAUMA |
|
|
 |
|
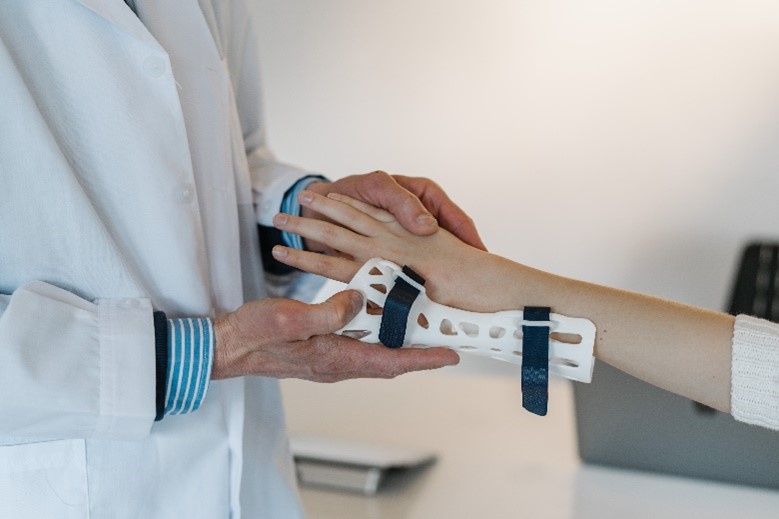
Despite the commonness of distal radius fractures, the optimal management strategy is still debated among surgeons. When the fracture is displaced, support of the bone fragments is necessary to hold the bone in position while it heals – this can be done with surgical implants (such as K-wires) or non-operatively with casts. With the current evidence on surgical fixation with K-wires being at high risk of bias, a large, high-quality RCT was needed to see whether surgical fixation is necessary, or whether casting can do the job.
The DRAFFT 2 Trial, conducted in 36 NHS hospitals in the UK, randomized 500 patients with dorsally displaced distal radius fractures to receive either a moulded cast (n=255) or the insertion of a K-wire (n=245) after manipulation of the fracture. The primary outcome of interest was wrist function, measured with the Patient-Rated Wrist Evaluation.
-
No significant differences in wrist function scores were observed between casting and K-wire fixation at 3, 6 or 12 months (p>0.05 for all).
-
No significant differences in quality-of-life scores between the two groups were observed at any time-point.
-
The odds of requiring surgical fixation due to loss of fracture position in the first 6 weeks was significantly higher in the casting group (OR 0.02 [95%CI 0.001, 0.100], p<0.001).
Bottom line. This study found no evidence of superiority with K-wire fixation compared to casting for distal radius fractures, suggesting that casting can be an effective (and affordable) solution. However, opting for casting may require future surgical fixation operations in some patients.
Check out the comprehensive analysis of this paper in our ACE Report. |
 |
|
|
|
|
 |
|
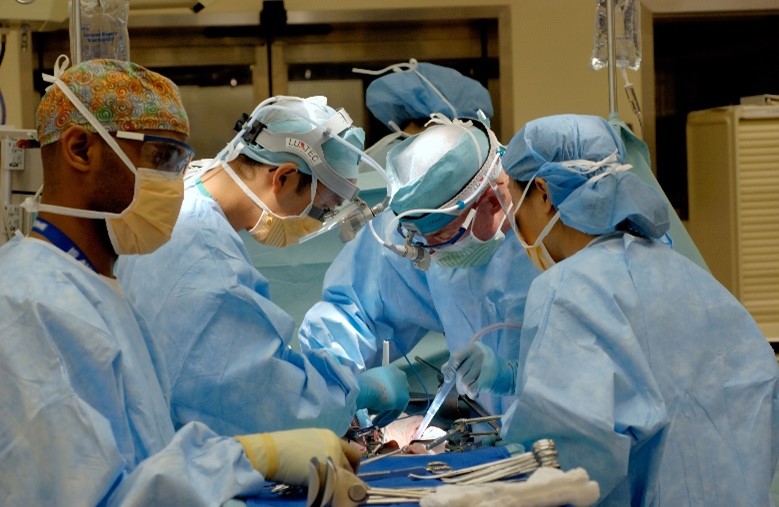
Dislocation is a major concern after revision total hip arthroplasty (THA). To minimize instability and the risk of dislocation, dual mobility implants have been widely used by surgeons. However, dual mobility implants have been reported to be prone to intraprosthetic dislocations – some suggest that a large femoral head in a conventional bearing could provide similar outcomes, but the evidence is limited and inconclusive.
Researchers from the United States recently conducted an RCT randomizing patients to either a dual mobility implant or a large femoral head implant. The primary outcome of interest was the rate of prosthetic dislocation, with secondary outcomes being revision and re-admission rates.
The results of the interim analysis were reported in the Journal of Arthroplasty:
-
There were no differences in the rate of dislocations between the large femoral head and dual mobility implant groups (p=0.67). The time to dislocation, however, was shorter in the large femoral head group (p=0.003).
-
No difference in the rate of revision (p=0.31) or the rate of 90-day re-admission (p=0.71) were observed.
Bottom line. The interim analysis results suggest no difference in the risk of dislocation between dual mobility and large femoral heads in revision THA. Continued follow-up will provide the full picture on this important question!
Check out the comprehensive analysis of this paper in our ACE Report. |
 |
|
OSTEOARTHRITIS |
|
|
 |
|
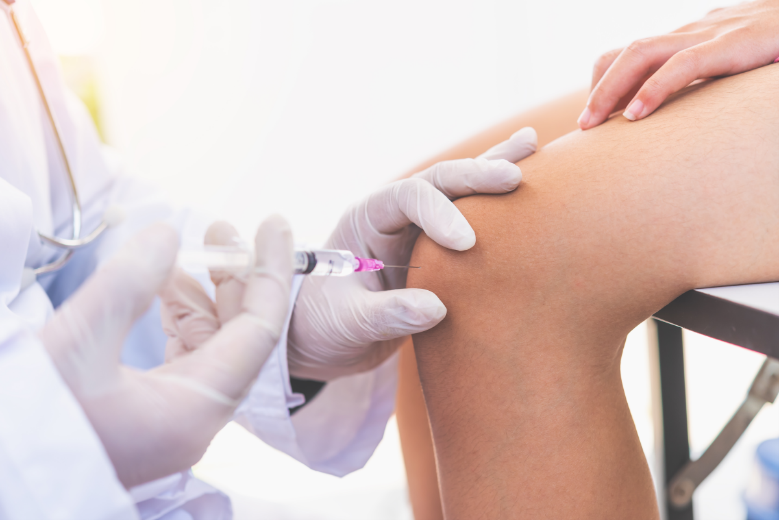
The prevalence of osteoarthritis is estimated to be over 500 million people globally. With aging populations poised to increase this number in the coming decades, effective non-operative and operative management strategies will be essential. One of the most popular (and divisive) interventions at the moment is platelet-rich plasma (PRP). While some swear by it, others are skeptical of its efficacy – we did a deep dive into the literature on PRP to see what the evidence says.
Using our state-of-the-art Surgical Analytics database, we analyzed the existing high-quality literature on PRP. Here’s what we found:
A Rise in Popularity. PRP injection use has quadrupled in the last 10 years and is set to grow even more. This is reflected in our readership: two of the top 3 most read OE articles in the last 4 years were PRP-related.
Academic Market Analysis. The global PRP market is expected to hit close to 2 billion USD by 2030. The Market Analysis tool identified the companies pumping the most time and resources into PRP research. Regen Lab from Switzerland and TCM Biotech are the two companies with the biggest share of the academic market. Interestingly, much of the existing PRP research has come from the East, in countries like China, Iran and Turkey.
Clinical Effectiveness. We ran a meta-analysis of RCTs using our database of over 160 million data points. We found that the current research suggests PRP to be superior to saline, hyaluronic acid, and corticosteroid injections, with no marked increase in the risk of adverse events.
Bottom line. PRP appears to be a promising treatment for knee osteoarthritis, with evidence of superiority over other injectable treatments like hyaluronic acid and corticosteroids. However, the current literature is limited and heterogeneous in quality – time (and future studies) will tell whether it will live up to the hype.
Read the full OE Insight on PRP for knee osteoarthritis.
|
 |
EDITOR’S PICKS |
|
|
|
Risk of Bias 2.0 – The assessment of study quality through risk of bias has become an essential component of systematic reviews. The Cochrane Risk of Bias 2.0 the gold-standard assessment tool for randomized controlled trials. (Read More) |
|
|
|
The Current State of AI in Medicine – For all of the intrigue surrounding artificial intelligence, there is growing pushback by many in the medical community who caution that current AI models are highly biased black box instruments with more promise than substance. In this Original, Dr. Joseph Silbert explores the promise and limitations of AI in medicine, emerging use-cases, and the implications of large language models (LLMs). (Read More) |
|
|
|
The OPAL Trial – One of 2023’s most influential trials in orthopaedics, the OPAL trial (published in The Lancet) found that opioids provided no advantage over placebo in patients with low back or neck pain, and actually led to slightly worse pain and lower quality of life. (Read More) |
|
|