|
|
|
|
|
|
|
|
 |
|
Adhesive capsulitis – or frozen shoulder – is regularly treated with corticosteroid injections. The single rotator interval injection has recently emerged as an injection site that provides good clinical outcomes for patients – however, there is limited data comparing it to multi-site injections. If multiple site injections are unnecessary, this could significantly reduce the cost and operation time associated with this treatment.
This randomized trial randomized 64 patients with primary frozen shoulder to receive a multisite triamcinolone acetonide injection (rotator interval; intra-articular; subacromial bursa) (n=32) or a single rotator interval injection (n=32). Outcomes of interest included pain, shoulder function, and patient satisfaction.
-
The multisite injection provided significantly greater pain relief at 4- and 8-weeks post-treatment compared to the single rotator interval injection (p<0.05 for both). No differences in pain scores at 12 weeks were observed.
-
Range of motion in flexion and abduction was significantly better in the multisite injection group up to 12 weeks post-treatment (p<0.05 for all). Internal rotation range of motion was also superior in the multisite injection group at 8 weeks (p=0.048).
-
Functional scores (ASES; Constant-Murley) were significantly better in the multisite injection group up to 12 weeks post-treatment (p<0.05 for all).
Bottom line. For patients with frozen shoulder, a multisite corticosteroid injection to the rotator interval, subacromial bursa, and intra-articular space led to significantly better clinical improvement compared to a single-site rotator interval injection.
Read the full ACE Report on this RCT here. |
 |
|
|
|
|
 |
|
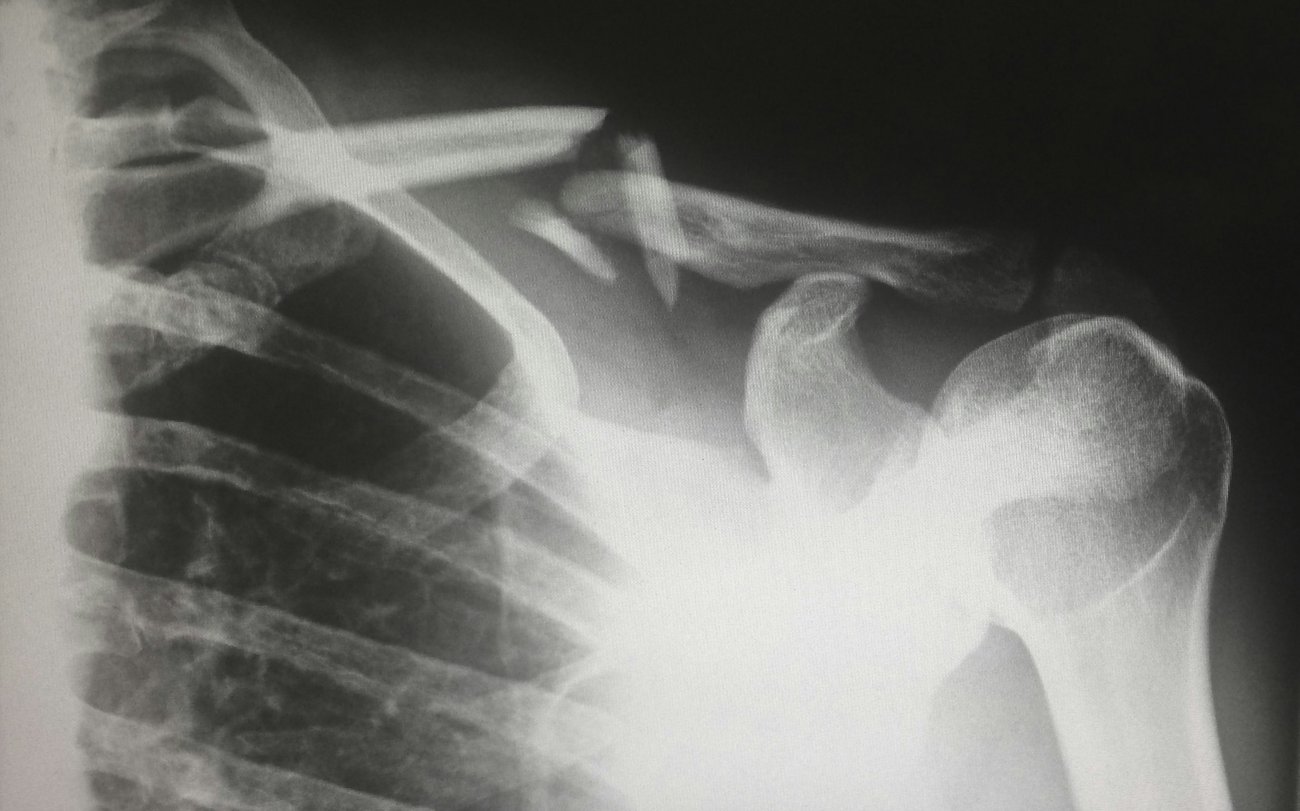
The vast majority of clavicle fractures occur in the midshaft. For surgical treatment, two fixation methods dominate: the intramedullary nail fixation and the plate fixation. The optimal treatment is still widely debated, particularly when it comes to wound complications. This systematic review and meta-analysis aimed to compare the existing evidence on the two methods.
11 studies with a total of 749 patients were included in this study, comparing wound infection, surgical incision length, operative time, dehiscence, blood loss, and length of stay.
-
The pooled analysis found significantly lower odds of wound infection in the intramedullary nail fixation group compared to the plate fixation group (p<0.0001).
-
The pooled analysis found intramedullary nailing to result in a shorter wound length, shorter operation time, less intraoperative blood loss, and a shorter length of stay compared to plate fixation (p<0.05 for all).
-
The pooled incidence of dehiscence was not significantly different between groups.
Bottom line. Intramedullary nailing could provide significant advantages over plate fixation for the treatment of midshaft clavicle fractures, reducing infection risk and improving peri-operative parameters.
Read the full ACE Report on this meta-analysis here. |
 |
|
|
|
|
 |
|
The cannulated screw is a popular and long-standing intervention for the treatment of femoral neck fractures. However, the operation is often done freehand, which is associated with limitations. Could a novel, laser-guided navigation system optimize surgical and clinical outcomes?
32 patients with femoral neck fractures were randomized to receive a cannulated screw fixation procedure using a newly designed laser-navigation device (n=16) or via the standard freehand technique (n=16). Surgical and clinical outcomes were assessed.
-
The laser group reported significantly shorter operative time, less radiation exposure, and less bleeding compared to the freehand group (p<0.001 for all).
-
The rate of first success was significantly higher in the laser group (93.3% vs. 60.0%, p=0.03).
-
No significant differences in pain scores, Harris Hip Scores, or fracture healing were observed between the two groups (p>0.05 for all).
Bottom line. This novel laser-guided navigation system for cannulated screw fixation in femoral neck fracture significantly improved the efficiency of the surgical procedure but did not lead to any advantage in clinical outcomes post-operation compared to the freehand technique.
Check out our full ACE Report on this paper. |
 |
EDITOR’S PICKS |
|
|
|
Basic Science as a Clinical Research Tool – In OrthoJoe Episode 81, Dr’s Marc Swiontkowski and Mohit Bhandari discuss the value of basic science research for contributing to clinical decision-making, and what to consider when applying the biomechanical studies in your own practice. (Watch) |
|
|
|
The Economics of Robotic Surgery – In this webinar, we sat down with Dr. Jean-Eric Tarride – one of Canada’s top health economists – to discuss the importance of economic evaluations for healthcare technologies, the concept of cost-utility and quality-adjusted life-years (QALYs), and the best practices for assessing robotic-assisted surgical systems. (Read) |
|
|
|
|