|
10 April 2024 | Volume 1 Issue 33 |
|
|
|
|
|
|
|
|
|
|
|
 |
|
Ankle fractures are a common occurrence – comprising approximately 10% of all fractures. Conventional surgical treatment involves open reduction and internal fixation of the medial malleolus. However, in light of soft tissue and implant-related complications, recent literature has explored nonoperative management of well-reduced medial malleolus fractures. This study aimed to address a gap in knowledge regarding the superiority of internal fixation compared to non-fixation in anatomically reduced medial malleolar fractures after fibular stabilization.
154 adult patients with closed, unstable bimalleolar or trimalleolar ankle fractures requiring surgery were randomized in a prospective clinical trial. The patients were allocated to either internal fixation (n=78) or non-fixation (n=76) of the well-reduced medial malleolus fracture after fibular stabilization. The primary outcome was the Olerud-Molander Ankle Score (OMAS), a measure of function, at 1-year post-randomization. Secondary outcomes included ankle and health outcome scores, such as the EQ-5D, complications, return to work or activities, and radiographic assessments.
-
No statistically significant difference was found for the primary outcome (OMAS at 1 year) between the fixation and non-fixation group (P=0.17).
-
There was a significant favorable EQ-5D score result for the fixation group (P=0.05), though clinically irrelevant.
-
Overall complication rates were comparable between groups.
-
The non-fixation group showed a notable 20% radiographic nonunion rate as compared to the fixation group (p<0.001), with a low rate of symptomatic cases requiring surgical reintervention.
-
All remaining outcomes, such as return to work or activities, and radiographic assessments, demonstrated a lack of statistically significant difference between groups at all time points.
Bottom line. Non-fixation of well-reduced medial malleolar fractures after fibular stabilization is a valid treatment option for unstable ankle fractures, especially if the fracture is anatomically reduced. However, clinicians should be aware of the 20% nonunion rate in the non-fixation group, even though the reintervention rate for symptomatic cases was low.
Read the full ACE Report on this study here. |
 |
|
|
|
|
 |
|
Now we have a very simple intervention that’s in every hospital, at your fingertips.
Gerard Slobogean
In this OrthoJoe podcast, Mo & Marc were joined by the lead investigators of the PREPARE Trial. Published in the New England Journal of Medicine, the PREPARE Trial found that iodine-in-alcohol antiseptic solution significantly outperformed chlorhexidine-in-alcohol solution for preventing surgical site infection in closed extremity fractures.
Listen to the entire podcast here.
|
 |
|
|
|
|
 |
|
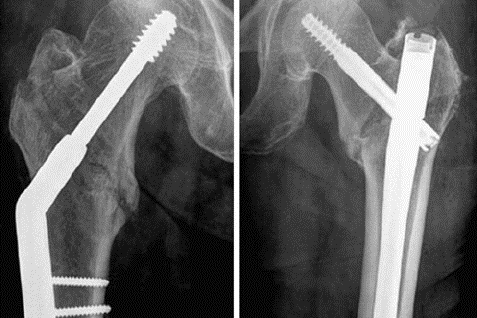
Proximal femur fractures are increasingly common among the elderly population and can lead to significant morbidity and mortality rates. Surgical treatment is the gold standard approach for hip fractures, with the intramedullary nail (IMN) and dynamic hip screw (DHS) being the most commonly used procedures. Despite extensive literature on the biomechanical advantages of both, there are inconsistent findings regarding the comparison of their postoperative clinical outcomes. This study provides a comprehensive analysis of the relative parameters and differences between IMN and DHS treatments in traumatic hip fractures.
Thirty randomized controlled trials with a total of 6,650 patients who sustained hip fractures classified as AO/OTA31A1-A3 were included in this systematic review and meta-analysis comparing surgical fracture fixation with IMN versus DHS. Pooled outcomes of interest included intraoperative differences such as blood loss and screening time, postoperative differences including hospital stays, time to healing, Harris score as well as complications such as femoral neck shortening, non-union, and femoral fractures.
-
A significant difference between IMN and DHS was found with regards to intraoperative parameters such as blood loss and screening time (P<0.0001).
-
IMN was advantageous in preventing femoral neck shortening (P<0.05) and non-union, however, its shortcomings are open reduction of the fracture and an increased risk of femoral fractures (P<0.0001).
-
In terms of the postoperative outcomes (hospital stay, time to healing, Harris score, and mobility score) and complication outcomes, there were no significant differences between the two treatment options.
Bottom line. While IMN may offer benefits in terms of blood loss, lower incidence of femoral neck shortening, and improved non-union rates, it is recommended to pay special attention to the risk of femoral fractures during IMN insertion.
Read the full ACE Report on this study here. |
 |
EDITOR’S PICKS |
|
|
|
What is Value Based Healthcare – In World Tour session, Dr. Rudolph Poolman explains how a value-based healthcare project on hip osteoarthritis, run in a group of seven teaching hospitals in the Netherlands, implemented the best available evidence on post operative restrictions. (Watch) |
|
|
|
David Parker: 10 Things About Me You Likely Don't Know – In this edition of Surgeon Features, we sat down with Dr. David Parker, director and founder of the Sydney Orthopaedic Research Institute & current President of ISAKOS. David shares his amazing insights on his journey to becoming a surgeon, his love for family, how to get through a daunting email backlog, and advice for early career individuals. (Read) |
|
|
|
|
|
|
|
|
PS. Enjoying The Pulse? Make sure to move it to your primary inbox so you don't miss it!
Any topics you would like to see covered?
Send your ideas to info@myorthoevidence.com
|
|
|
|
|
|
|
|
|
This email was brought to you by OrthoEvidence |
|
|
|
|