|
|
|
|
|
|
|
|
 |
|
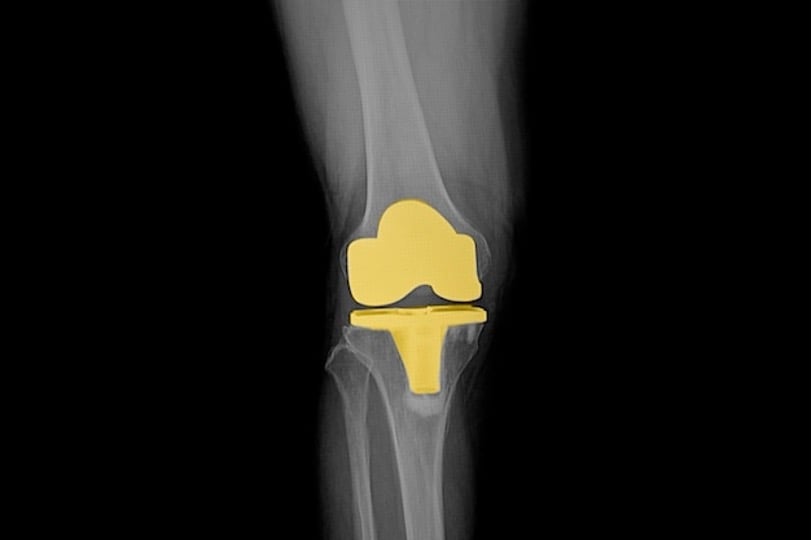
Knee osteoarthritis is one of the most common chronic conditions in orthopaedics, with total knee arthroplasty (TKA) being the gold-standard intervention for end-stage cases. There is growing interest in different tibial baseplate fixation methods in younger patients. This study aimed to compare long-term outcomes and survivorship of cemented tibial components, pegged porous cementless tibial components, and tantalum monoblock porous tibial components.
224 patients with knee osteoarthritis were randomized to receive different tibial baseplate fixation methods during total knee arthroplasty (TKA). The patients were assigned to three groups: Group 1 received a cemented tibial component (n=97), Group 2 received a pegged porous cementless tibial component (n=87), and Group 3 received a cementless tantalum monoblock porous tibial component (n=90). The primary outcome of interest was survivorship, and secondary outcomes included functional measures (such as the Oxford Knee Score & Knee Society Score) and radiological data. Outcomes were assessed up to 10 years postoperatively.
-
Irrespective of the tibial component, functional and radiological outcomes remained similar for up to 10 years post-operation.
-
Survivorship was excellent across all groups (99.6%).
-
Differences in functional outcomes were not statistically significant between groups.
-
Radiological and survival outcomes were similar in all three groups.
Bottom line. The study suggests that the long-term outcomes and survivorship are likely to be satisfactory in patients undergoing total knee arthroplasty, regardless of the choice of tibial component. Up to 10 years, the fixation method may not significantly impact the 10-year outcomes.
Read the full ACE Report on this trial here. |
 |
|
|
|
|
 |
|
In this edition of Surgeon Features, we sat down with Dr. David Parker, director and founder of the Sydney Orthopaedic Research Institute & current President of ISAKOS.
David shares his amazing insights on his journey to becoming a surgeon, his love for family, how to get through a daunting email backlog, and advice for early career individuals.
“I think one thing I haven't really discussed are the sacrifices made on other aspects of life, especially the impact on family, and the uncertainty around whether it's all worth that cost. I love my career and what I have been able to achieve, but I'm not sure if I'll ever know if I got that balance right.”
Read the full interview here. |
 |
|
|
|
|
 |
|
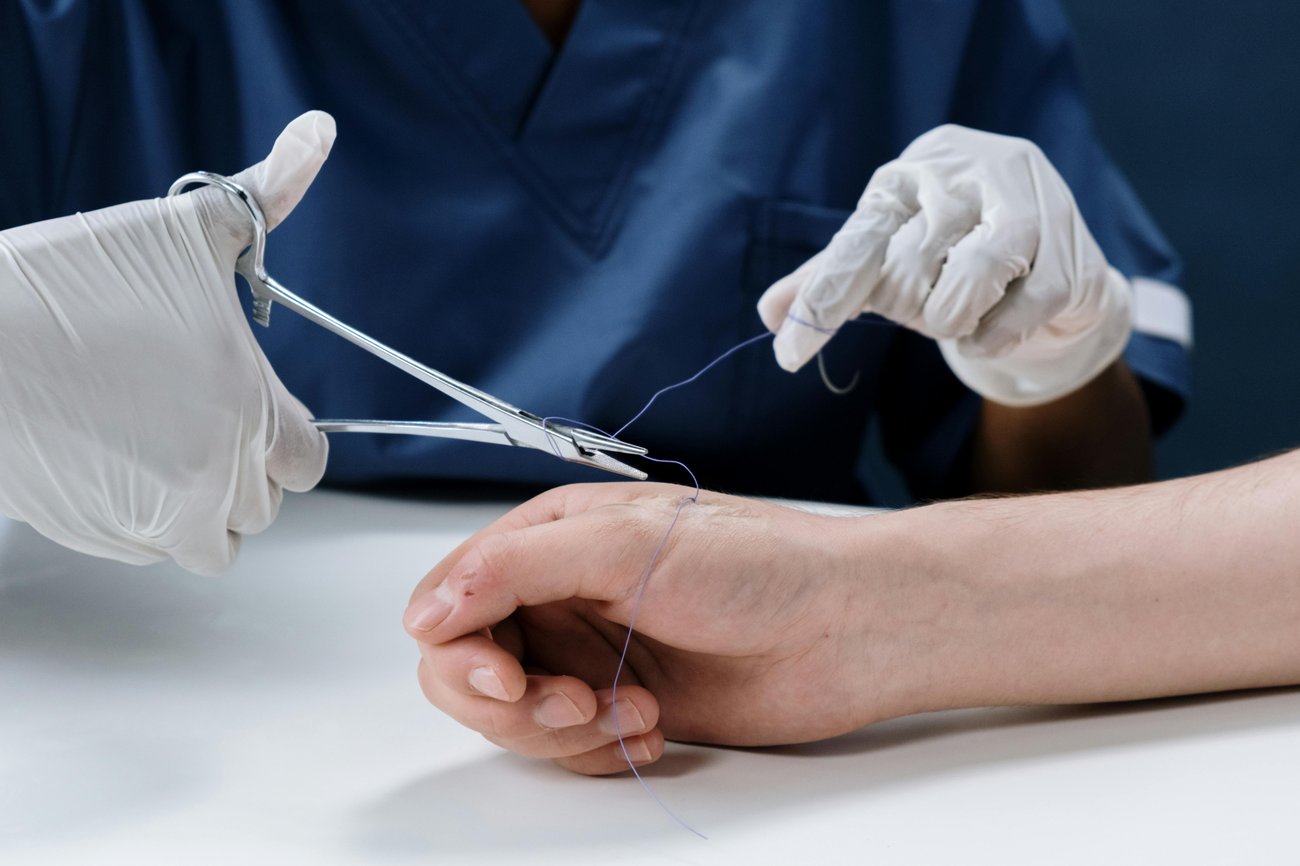
Carpal tunnel syndrome results from chronic median nerve compression; when conservative treatment is unsuccessful, surgery is often the next option. There has been ongoing debate regarding the optimal approach to wound closure after open carpal tunnel release surgery due to a lack of definitive evidence on wound healing, appearance, and patient satisfaction. This study sought to compare the effectiveness of two common methods: interrupted, buried Monocryl sutures and traditional nylon horizontal mattress sutures.
125 patients undergoing an open carpal tunnel release procedure were randomized to receive either interrupted, buried Monocryl sutures or traditional nylon horizontal mattress sutures. Primary outcomes focused on scar assessment using the Patient and Observer Scar Assessment Scale (POSAS) questionnaires which were completed at 2 and 6 weeks postoperatively.
-
Patients and observers rated scars closed with Monocryl sutures more favorably compared to nylon sutures at 2 weeks (P<0.01).
-
By the 6-week follow-up post-surgery, no significant differences existed between the two groups in terms of scar ratings by both patients and observers
Bottom line. Early postoperative scar appearance and patient satisfaction favor Monocryl sutures, suggesting potential benefits for optimizing patient perception during the initial critical recovery period. However, these differences diminish over time, and long-term outcomes may not differ substantially between Monocryl and nylon closures.
Read the full ACE Report on this trial here. |
 |
EDITOR’S PICKS |
|
|
|
Misconceptions About DEI and How to Measure Success in Equity Work – In OrthoJoe Episode, Dr’s Marc Swiontkowski and Mohit Bhandari sit down with special guest Dr. Saroo Sharda, Associate Dean of Equity and Inclusion at McMaster University and Equity, Diversity and Inclusion (EDI) Lead at the College of Physicians and Surgeons of Ontario, to discuss her journey into the field, common misconceptions about EDI, and how to measure success in equity work. (Watch) |
|
|
|
Mini-Masters: Linear Regression – Statistics is the tool by which we assess the data from our studies. One of the most powerful statistical methods used in practice is linear regression. Whether you are identifying factors associated with prosthesis alignment or predicting treatment effectiveness, linear regression has powerful use cases for the surgical scientist. In this Original, we explain the inner workings of a linear regression model, its strengths, limitations, and assumptions, examples of its application in the real-world, and how you can conduct your own! (Read) |
|
|
|
|